NHS workers take tips from the performing arts to improve workplace wellbeing
A multidisciplinary partnership in Wales has transferred knowledge from the performance arts to NHS staff members' mental health and wellbeing.
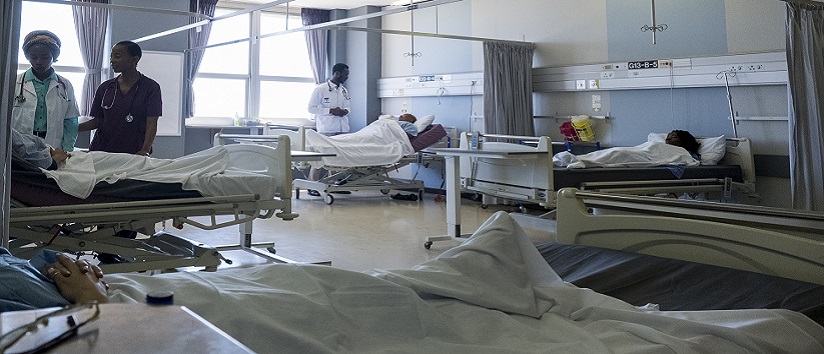
NHS staff members have been exposed to the forefront of Covid-19; hospital wards have overflowed, and workplace burnout has become yet another symptom of the pandemic.
The annual NHS Staff Survey revealed the extent of the mental toll of the last year; 44% of NHS staff members reported feeling unwell because of work-related stress, and more than one in four are thinking about leaving their NHS organisation altogether.
In the landscape created by the virus, new techniques for coping with work-related stress has become ever more vital to help staff members maintain their mental health and continue to compassionately engage with patients and colleagues despite restrictions.
- See also: 'Workplace mental health – the flight over the cuckoo’s nest'
- See also: 'One year on, it is clear that despite adversity, our NHS delivered'
Performing Medicine – supporting healthcare professionals through challenging times
The charity Clod Ensemble has announced the success of an innovative pilot programme that utilised techniques used in the performing arts to improve staff wellbeing and mental health.
Delivered by Performing Medicine in collaboration with Swansea Bay University Health Board (UHB) and Swansea University, the arts-based sessions encouraged self-care and promoted communication between staff members to help them better cope with work-related stress.
More than 80 staff members participated in the interactive workshops that inspired healthcare professionals to think about, practice, and demonstrate high-quality care through techniques such as breathing exercises, spatial awareness, and improv.
Jo Mclean, executive director at Performing Medicine, said: “As Covid-19 accelerates collaboration between the arts and healthcare, arts-based interventions to increase staff mental health and wellbeing are increasingly being used in the NHS. High levels of stress among healthcare workers is common, and Performing Medicine is very proud to collaborate with Swansea Bay University Health Board and Swansea University to support healthcare professionals to continue to deliver their invaluable work by helping to improve their mental health and wellbeing.”
Ms Mclean added: “The workshops are about team building, resilience, and managing their own stress and wellbeing. I think there are lots of crossovers for lots of different businesses, particularly in terms of how you work in teams and how you communicate with people effectively.”
“We might concentrate on breath work or using techniques that performance has used over many years to prepare themselves, and then translating into how we would work with healthcare professionals to prepare themselves both mentally and physically.”
Absenteeism has been a particular problem for the NHS during the pandemic, as staff members contract the virus or require time off to recuperate their mental health after long stressful shifts. Prue Thimbleby, arts in health coordinator, Swansea Bay UHB, commented that there had been a noticeable decline in absenteeism since the workshops were trialled last year, “we've been trying for years to solve the staff sickness problems, and if this is making a difference. Let's go, let's do more of it.”
She continued: “The arts have got a massive amount to offer healthcare. And I think it just takes a bit of lateral thinking to see that healthcare has got some entrenched problems that we've been trying to solve for decades, and the arts brings something fresh that might provide the solution that we've been looking for.”
- See also: 'Public Health England launched free three-week children’s mental health training course'
- See also: 'A severe shortage in hospital beds is leaving patients without treatment'
“Perhaps we didn’t realise the pressures we're working under and realise how it makes a difference in your character”
Aside from reducing staff shortages, the pilot programme results also strongly demonstrated that it helped staff cope better with the demands of the job, be more confident in their work, and communicate with patients and colleagues in a more attentive way. Also, the reported outcomes indicated an increased awareness of the importance of making time for self-care and how non-verbal behaviour and posture affects the wellbeing of those around them.
Andrea Bradley, a lead nurse at Swansea Bay UHB, said that the sessions had “given me that time to connect with my mental health as well and meet people that we would never have met with before”.
She described her experience: “There were three actors on the stage, one dressed as a nurse, a ward receptionist, and a patient. And they are acting on the stage on us; as the audience, we were stopping them, for example, by saying, ‘don't speak to your board manager like that’. And the actors would say to the audience, ‘okay, how should I speak to the ward manager, then?’ … And by the end, we had a perfect scenario and the perfect outcome for the patient.”
Ms Bradley continued that the experience had improved workplace communication and also has had a profound impact emotionally on her and her colleagues:
“We've been through a lot together over the last year – we've watched each other work our fingers to the bone… Perhaps we didn’t realise the pressures we're working under and realise how it makes a difference in your character – having to deliver day in day out. It changes your character; it changes the way you communicate with people.”
“Seeing the difference between the staff from the morning when they first meet Performance Medicine to five o'clock when we finish is absolutely mind-blowing. The change in my personality from working with Performing Medicine, from then to now is massive, absolutely massive; I'm far more open with people now and are far more likely to tell people how I feel”, she added.
Comments
Write a Comment
Comment Submitted